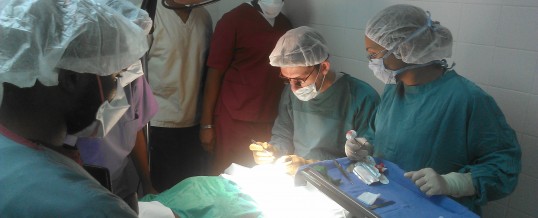
I returned to Port-au-Prince in early January to continue our mission of training the residents at the State University Hospital. I was able to coax my brother Tom, an anesthesiologist in Colorado Springs, to accompany me. Normally, we do 90% of our cases with only local anesthesia and save the most invasive for the main OR, where general anesthesia is available. The problem is, the turnover time between patients was upwards of 90 minutes, meaning we could only do a half dozen cases in a day. They usually only allowed us in there for one day during the trip, so many patients just simply couldn’t be treated. Well, last year the ophthalmology department received an old anesthesia machine and Tom came along to run it and give some comfort to our patients. He was masterful at getting the patients asleep with minimal resources, and then turning over the bed in around 20 minutes.
This made our challenging cases suddenly manageable. It is hard to describe how you feel as a surgeon operating in these types of places. The instruments are very poor, the lighting is non-existent, the cautery is archaic (meaning lots of bleeding going on). So to at least have a patient that isn’t squirming and moaning through the procedure makes the job so much easier.
We saw some real challenges. A few memorable patients with advanced tumors showed up needing care. This woman in the photos below had an orbital tumor growing for 3-4 years, which eventually forced her eye clear out of the socket. She couldn’t afford a CT scan, so we had no way of knowing the extent of the tumor or if it extended into the brain. My plan was to just remove the blind eye so that she would be more comfortable and then assess the tumor manually. With the eye removed, I felt a large, firm mass filling the eye socket. I carefully probed around it and spent about 20 minutes probing it to see if it would move. Once I felt confident that it was well encapsulated and limited to the eye socket, I maneuvered it out. It was about the size of an egg. A tumor this size would almost never be seen in the US as people can get treatment before things get too far advanced. The final photo at the bottom right shows her socket with an implant, closure of the soft tissues inside the eyelids and a plastic conformer where her artificial eye will eventually be placed.
A second tragic case involved a man with a rapidly growing tumor on his right eye (top 2 photos below). This growth had started last summer and blossomed into a massive growth, which had totally destroyed his eye. Getting around a tumor like this is extremely difficult. The bleeding was severe and the tissue fell apart with every touch. I finally managed to get it out, along with most of the contents of the eye socket. Thankfully it spared his eyelids and they could be closed directly. The second gentleman had a large skin cancer involving the lower eyelid and nose, which was removed and reconstructed with a combination of sliding skin flaps.
As always, the kids in Haiti are the real treat. I haven’t seen an ugly baby down there. They don’t exist. The parents are so concerned and attentive. Most have tearing problems or small wounds that need to be revised. A few come in with advanced tumors, many of which are beyond what can be safely operated on in that setting.
We had a great time with the residents and staff at the hospital. They work hard to accommodate us and keep the sutures and hot instruments coming. We look forward to our next trip.
JAN

About the Author:
Dr. Matheson Harris is an oculofacial plastic surgeon and ophthalmologist in Salt Lake City, Utah.